How ovarian cancer is treated may vary between hospitals and doctors, but overall treatment plans are based on:
- The stage of the cancer
- The grade of the cancer
- The type and size of the tumour
- Your age and general health
- Whether the cancer has just been diagnosed or has recurred
Surgery
Surgery is often the first step in treating most ovarian cancers. For some, treatment may begin with chemotherapy to shrink the tumour before surgery. This is called neoadjuvant chemotherapy.
Surgery is also important for staging the ovarian cancer. When the tumour is removed through surgery it will be examined by a and the stage and grade of the ovarian cancer will be determined. This will help the gynecologic oncologist determine the appropriate treatment.
How surgery is performed
Surgery for ovarian cancer should be performed by a gynecologic oncologist.
A gynecologic oncologist is a medical doctor with five years of postgraduate training in obstetrics and gynecology plus an additional two years of cancer training. When surgery is performed by a gynecologic oncologist the chances are improved for a longer time to possible recurrence and increased survival time.
The standard treatment for ovarian cancer is of the cancer: the surgeon removes as much of the tumour as possible. Ideally the patient should be reduced to no visible as maximal debulking has been shown to improve a prognosis.
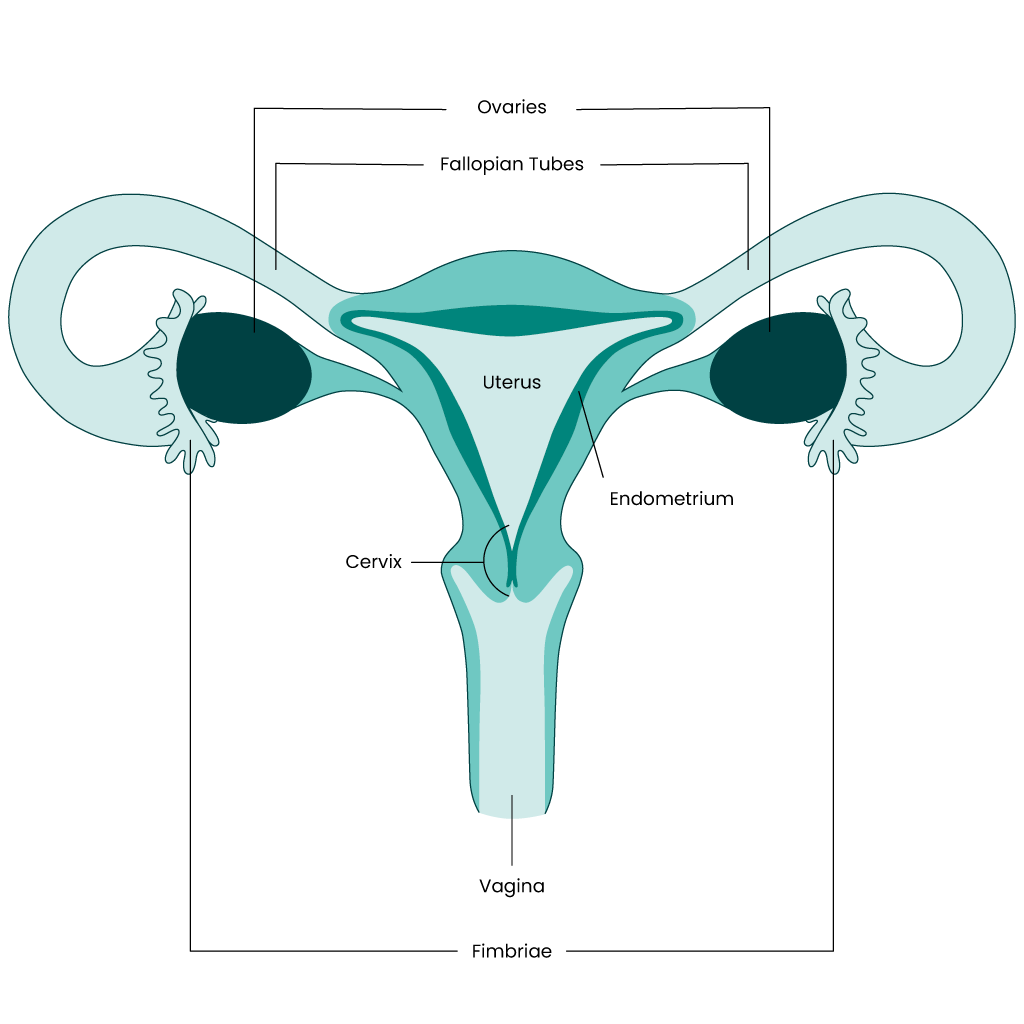
In most ovarian cancer surgeries, the surgical team will remove the uterus, both fallopian tubes, and both ovaries. The clinical name for this type of surgery is “total with ”.
In some cases, the surgical team may put a flexible tube, called a “port” into the abdominal wall so that chemotherapy can be administered directly into the abdominal cavity. This is called “IP chemotherapy”.
After the surgery
Always ask your doctor or the nurse assigned to you to explain what has been removed and anything that is not clear about the surgery. Be sure to also ask about the type of ovarian cancer you have, the stage, and the grade.
After surgery for ovarian cancer, your gynecologic oncologist is likely to recommend chemotherapy and/or radiation; chemotherapy may also be given before surgery (neoadjuvant chemotherapy).
In some cases, chemotherapy may not be needed because the cancer was caught at an early stage and therefore it is unlikely to come back (recur).
Recovery period
Recovery may take about 6-8 weeks, depending on a number of factors such as: your general state of health prior to surgery, the extent and complexity of your surgery, and how much rest you are getting.
Assuming you have no serious complications such as infection, you will normally go home within a week after the surgery.
Some side effects of surgery may include:
- Vaginal bleeding or discharge
- Urinary tract frequency and urgency
- Incision problems
- Gastrointestinal problems
- Fatigue
- Decreased libido
- Increased feelings of stress, anxiety, and/or depression
- Pain and swelling
- Rash or itching
Talk to your healthcare team if you are experiencing any of these side effects.
Continue learning
Resource guide
Self care after surgery
It is important to be gentle with yourself following surgery for ovarian cancer. Here are some activities that might help you to feel better, and some activities that you may want to avoid.
Video
Managing the Side Effects of Treatment
Treatment for ovarian cancer is associated with a range of side effects. Learn about common side effects and importantly, find out how you can effectively treat and reduce them.
Chemotherapy
Chemotherapy literally means “to treat disease with chemicals”. There are many different types of chemotherapy protocols for ovarian cancer.
Your treatment will depend on the type of ovarian cancer and the stage (how far it has spread). Chemotherapy or “chemo” is the use of one drug or, usually, a combination of drugs to kill cancer cells throughout the body. Chemotherapy affects the whole body rather than just one part of it.
- Chemotherapy is often used as a treatment for ovarian cancer, either before or after surgery.
- Given before surgery (neoadjuvant chemo), the chemo reduces the size of the tumour, making it easier to remove.
- After surgery (adjuvant chemo), the chemo is used to destroy any remaining cancer cells.
Chemotherapy drugs
Chemotherapy to treat ovarian cancer typically includes a combination of two different chemotherapy drugs.
The first drug is usually a , either “cisplatin” or “carboplatin”. The second drug is usually a , either “Taxol” or “Taxotere”. Other chemotherapy agents may be used to prolong survival.
How chemotherapy is performed
By IV
Chemotherapy drugs are injected into a vein (given ‘intravenously’ or IV) so that they can circulate through the bloodstream.
By IP therapy
‘Intraperitoneal’ chemotherapy or IP chemotherapy is used for stage 3 and 4. The drugs are given straight into the abdomen through a plastic tube.
By mouth
Some chemotherapy treatments are given by oral tablet.
Continue learning
Resource guide
Managing side effects of chemotherapy
Chemotherapy commonly produces many side effects, get tips on how to manage them.
Video
Managing the Side Effects of Treatment
Treatment for ovarian cancer is associated with a range of side effects. Learn about common side effects and importantly, find out how you can effectively treat and reduce them.
Radiation
Radiation therapy can be used to treat some cancers. It uses a very high dose of radiation to destroy cancer cells and damage the DNA of the cancer cells so that it can no longer divide and grow. Radiation therapy may be used if there is no or minimal residual cancer left after debulking surgery or if ovarian cancer recurs.
Side effects may include:
- Fatigue
- Mild redness/skin sensitivities
- Loss of appetite
- Hair loss in the pelvic region
- Nausea and vomiting
- Diarrhea or constipation
- Gas
- Bladder problems (frequent urination, discomfort, bleeding)
- Treatment-induced menopause
- Vaginal irritation
- Low blood counts
- Sexual changes
These problems will fade once radiation therapy ends.
Continue learning
Video
The 411 on sexual changes after cancer | Ovarian Cancer Canada Speaker Series
Do you have questions about sex and your sexuality after a cancer diagnosis? In this session, get the 411 on sexual changes after cancer with Dr. Anne Katz, certified sexuality counselor and Clinical Nurse Specialist at CancerCare Manitoba.
Video
Managing the Side Effects of Treatment
Treatment for ovarian cancer is associated with a range of side effects. Learn about common side effects and importantly, find out how you can effectively treat and reduce them.
Medications to treat ovarian cancer or prevent a recurrence
PARP inhibitors
inhibitors are a category of drugs that can be used to treat new and recurrent ovarian cancers. PARP inhibitors are taken orally (in pill or capsule form). When prescribing a PARP inhibitor, your oncologist will take many aspects of your unique case into consideration, including whether or not you have certain genetic mutations. PARP inhibitors available in Canada include:
- Olaparib (brand name: Lynparza)
- Niraparib (brand name: Zejula)
Bevacizumab
Bevacizumab (sometimes called “bev”) belongs to a group of drugs called “angiogenesis inhibitors”. This means that bevacizumab prevents (or “inhibits”) cancer cells from being able to make new blood vessels, therefore slowing or stopping the cancer growth.
Bevacizumab is given intravenously, meaning that it is injected directly into the vein.
The bevacizumab in Canada is called “Bambevi”.
Other therapies
Complementary therapies
Offered in addition to traditional treatments, most complementary therapies methods are NOT offered as cures for cancer but they are used to help you feel better. They might include wide ranging activities such as meditation to reduce stress or ginseng to assist with fatigue.
Recommendation
Some complementary methods through studies are known to help, while others haven’t been tested. It is recommended that complementary therapies be done in consultation with your oncologist.
Alternative treatments
Alternative methods may be offered as cancer cures, in place of traditional treatment, however they haven’t been proven safe and effective in clinical trials.
Recommendation
Always discuss any alternative therapy with your doctor prior to embarking on a course of treatment as untested therapies may have limited effect on your ovarian cancer and experimenting with unproven therapies can be harmful.
Australian Cancer Council (2021). Taking care of yourself at home after surgery. Retrieved: https://www.cancercouncil.com.au/ovarian-cancer/treatment/surgery/taking-care-of-yourself-at-home-after-surgery/
Canadian Cancer Society (2022). Lymphedema. Retrieved: https://cancer.ca/en/treatments/side-effects/lymphedema#ci_lymphedema_89_4458_00
Canadian Cancer Society (2022). Radiation therapy. Retrieved: https://cancer.ca/en/treatments/treatment-types/radiation-therapy
Canadian Cancer Society (2022). Radiation therapy for ovarian cancer. Retrieved: https://cancer.ca/en/cancer-information/cancer-types/ovarian/treatment/radiation-therapy
Canadian Cancer Society (2022). Surgery for Ovarian Cancer. Retrieved: https://cancer.ca/en/cancer-information/cancer-types/ovarian/treatment/surgery
John Hopkins Medicine (2022). The pathologist. Retrieved: https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/the-pathologist
May Clinic (2022). Low blood cell counts: side effects of cancer treatment. Retrieved: https://www.mayoclinic.org/diseases-conditions/cancer/in-depth/cancer-treatment/art-20046192
National Cancer Institute (2022). Intraperitoneal. Retrieved: https://www.cancer.gov/publications/dictionaries/cancer-terms/def/intraperitoneal
National Cancer Institute (2022). Platinum. Retrieved: https://www.cancer.gov/publications/dictionaries/cancer-terms/def/platinum
National Cancer Institute (2022). Taxane. Retrieved: https://www.cancer.gov/publications/dictionaries/cancer-terms/def/taxane


